Generally speaking, a laboratory diagnosis is of interest to both the individual and the community, as follows:
– establishing the microbial etiology of the sick at different disease stages, the prognosis and the efficiency of the given treatment;
– establishing the source and route of transmission of the pathogen involved;
– establishment of the carrier state with microbial pathogens or conditionally pathogenic agents;
– identifying inaparently / latent forms of disease;
– assessment of immune status.
Laboratory diagnosis in microbial pathology includes two ways of investigation:
A. DIRECT METHODS
Bacteriological (direct) diagnosis: – Detection of the pathogen, its components or a product (e.g. toxin) from the patient or the external environment.
Steps:
a. Collection and transport of laboratory samples.
In order to obtain a correct result it is necessary to observe the following preanalytical rules:
-the collection takes place as close as possible to the onset of the disease;
– sampling is done before antimicrobial treatment;
– use sterilized containers to prevent product contamination (use of standardized containers, such as hatchery, collection buffer, test tubes);
– the collected sample is properly carried out by the patient or medical staff to prevent contamination during collection;
-the product is properly labeled and transported to the laboratory under appropriate conditions.
Example:
Vaginal secretion
in cervicitis – muco-purulent leakage collection: remove mucus from the cervix – sterile compresses, with buffers (3) collect the pathological product by inserting and rotation into the cervical canal; Gram smear buffer 1, N.gonorrhea swab 2, Giems-C. trachomatis smear 3 buffer.
in vaginitis – secretion collection; from the vaginal bag bottom with sterile swabs (3) which are then placed in transport medium (do not refrigerate: N. gonorrhea dies); Buffer 1 – 0.5 ml isotonic saline solution 37 Celsius degrees then blade / lamella examination, Buffer 2 – Gram smear, Buffer 3 – Cultivation for Candida – and cultured for: N.gonorrhee, S. aureus, Streptococcus pyogenes, etc.
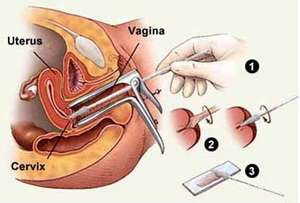
Sampling [Source]
- Macro-and microscopic examination (fresh preparation, fixed and coloured smear)-method for the orientation of the diagnosis – brings information about the presence of bacteria, the number, morphology and structure of bacteria, as well as their tinctorial characteristics (the ability of bacteria to fix different dyes).
Example:
- Fresh preparation between the blade and the slide:
-In urinary sediment: follows the presence of leukocytes, sedimentation, epithelial cells, crystals, bacterial flora, yeasts, cylinders, etc.

Smear made from pathological product or bacterial culture Gram stain [Source]
- Smear directly from the product:
-Gram Coloring: Highlight the presence of microorganisms, morphology (shape, size, characteristic layout), dyeing ability (gram + or Gram-), relationship with PMN (intra and extra leukocytes diplococci);
-Giemsa coloring: Allow Accurate visualization of cellular morphology, quantitative appreciation of the predominant PMN/assessment of inflammatory reaction, presence of anomalies/ cellular atypia /suspicion of neoplastic changes,
C. Highlighting of soluble bacterial antigens in biological liquids (blood serum, urine …) by serological methods
D. Detection of microbial DNA (hybridization reactions, Gene amplification – PCR)
- Isolation of germs in pure culture:
- Sowing and cultivation on cultured media
The sowing of pathological products is sterile, with bacteriological dropper, the exudate pad or Pasteur pipette, using sterile culture environments and adequate composition (ensuring optimal conditions for microbial development, growth and multiplication), on the surface or in depth, with the purpose of obtaining pure microbial cultures and isolated colonies.
- Inoculation in animal laboratory-method of isolation of bacteria in vivo (example: Pneumococcus or Klebsiella in mice)
- Identification of isolated germ from pure culture:
- Exam of cultural and morphotinctorial characteristics
-Morphological (Gram/AM smear (methylene blue)/from the colony),
-Culture characters: S/Smooth (creamy), R/Rough (rough), M (mucous, encapsulated), hemolysis, pigment, invasion etc.
- Biochemical and Metabolic character investigation – differentiates bacterial species on the enzymatic properties (viewed on a coloured substrate, by modifying PH, color change), inside of the genus, family, etc.
- Determination of the antigenic structure by:
Agglutination reactions
Precipitation reactions
Capsule swelling Reactions
- Determination of sensitivity to Bacteriophages (Lysotypia)
- Microbial DNA detection techniques-Methods of molecular biology/PCR techniques
- Determination of the pathogenicity of the germ isolated by:
- In vitro tests-identification of pathogenic factors (Ex: Free coagulase in Staphylococcus aureus); highlighting the effects of bacterial pathogenicity on cell cultures;
- In vivo tests-experimental infection in the laboratory animal
5. Determination of germ sensitivity/resistance to antibiotics and chemotherapy – antibiogram
B. Indirect methods
1. Sero diagnosis – Detection and titration of specific antibodies in the patient’s serum. Antibodies are followed in dynamic-they appear over 7-10 days after onset and often persist after healing.
2. Intradermal reactions (Biological skin reactions for diagnostic) – Occurrence of a local cellular reaction (erythema, infiltrated) 2-4 days after the epidermal or intradermally introduction of the microbial allergen.

